Contact Us
Contact Us
At Chrysalis Psychology & Wellbeing, we offer Cognitive Behavioural Therapy (CBT) as part of our evidence-based approach to treating anxiety, depression, trauma, stress, sleep difficulties, low self-esteem, and a wide range of other mental health conditions.
.svg)
You have been here before.
You know the feeling. You wake up and before your feet hit the floor, your mind is already rehearsing the worst version of the day. You play back a conversation from three days ago, convinced you said the wrong thing. You put off a phone call because something inside you says it will not go well. You feel it in your chest before anything has even happened.
It is not a character flaw. It is not weakness. It is a pattern. And your brain has been running it for so long, it has become automatic.
That is exactly where CBT begins.
Cognitive Behavioural Therapy is built on a deceptively simple idea: the way you interpret a situation shapes how you feel, and how you feel shapes what you do.
Think about what happens when you send a message and do not hear back. One person thinks nothing of it. Another spends the next hour wondering what they did wrong. The situation is identical. The experience is completely different. The difference is in the thought.
The trouble is that these interpretations are not always conscious. They are fast, habitual, and often invisible. CBT calls them automatic thoughts. They run underneath everything, colouring how you see yourself, other people, and the world around you.
When those automatic thoughts are frequently harsh, self-critical, or catastrophic, they create a cycle that is hard to escape from on your own. Your thoughts drive your feelings. Your feelings drive your behaviour. Your behaviour confirms your thoughts. Around and around it goes.
CBT helps you see that cycle clearly for the first time. And once you can see it, you can begin to change it.

CBT stands for Cognitive Behavioural Therapy. It is one of the most extensively researched psychological treatments in the world, recommended by the World Health Organisation and the Australian Psychological Society as a first-line treatment for anxiety, depression, and a wide range of other conditions.
It works by helping you notice the connection between your thoughts, feelings, and behaviour, and then developing practical skills to shift that connection in a healthier direction.
Unlike some other approaches, CBT is not primarily focused on the past. It is focused on what is happening right now. What are the thoughts that keep showing up? What are you avoiding? What patterns have become so automatic you have stopped noticing them?
It is structured, collaborative, and practical. You are not a passive participant. You work with your psychologist, not simply talk to them. You leave sessions with real tools you can use in real life.
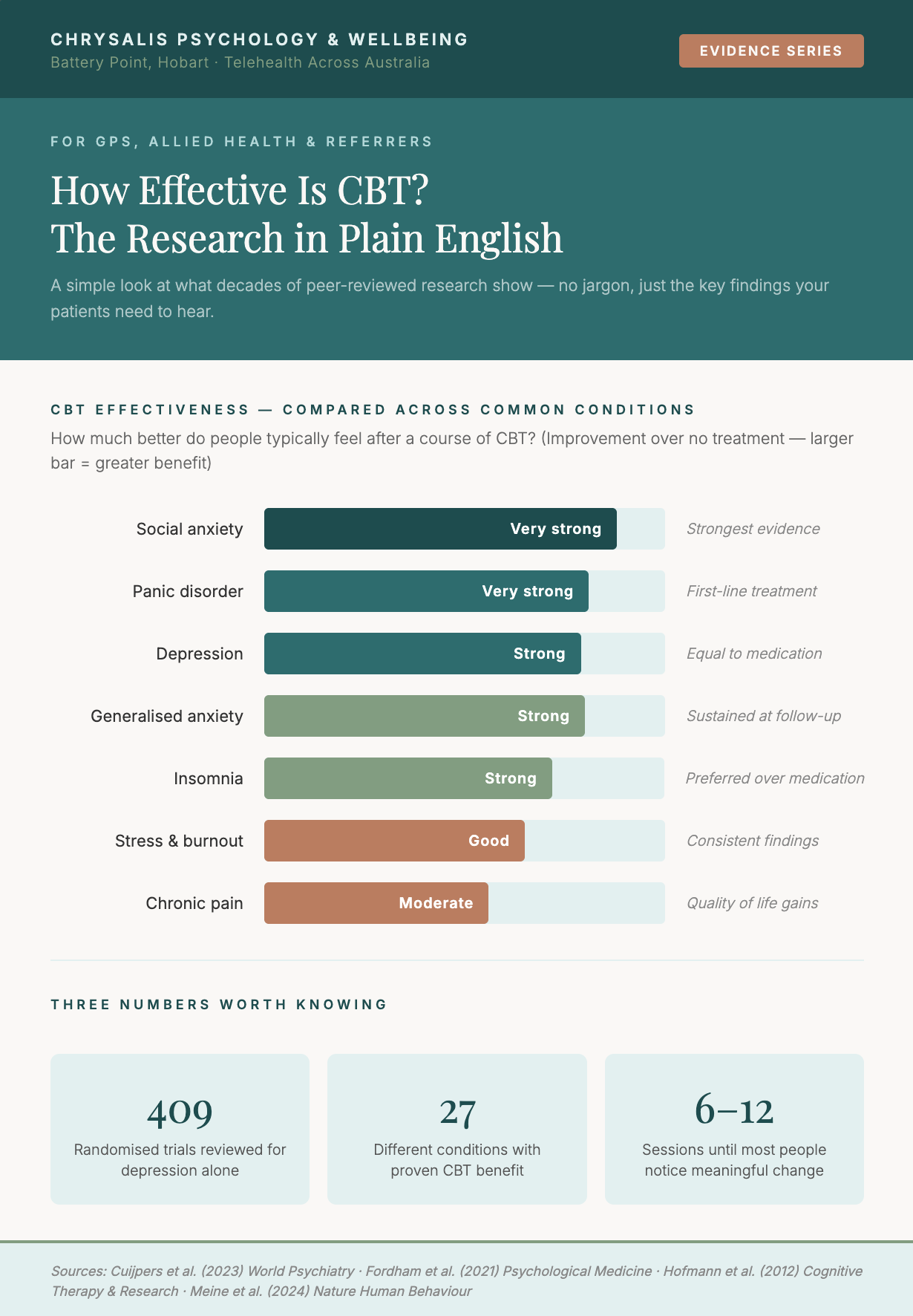
Research involving more than 52,000 patients across 409 independent trials has consistently found that CBT produces meaningful improvements in depression, with benefits that are maintained at six-to-twelve-month follow-up. Across 494 systematic reviews covering 27 different conditions, the evidence shows CBT produces consistent benefits for physical and mental health alike (Fordham et al., 2021, Psychological Medicine).

This is one of the reasons CBT is so widely used. The research supports its effectiveness across an unusually broad range of presentations. Our psychologists use CBT to help people with:
CBT is also one of the most well-researched treatments for children and young people. Our psychologists adapt CBT to be developmentally appropriate, using language and activities that make sense for younger clients. We also work with parents and caregivers were helpful, so families can support progress between sessions.
If you are imagining lying on a couch and discussing your childhood for years, that is not CBT.
CBT sessions are focused, practical, and grounded in what is happening for you right now. In a typical course of CBT, your psychologist will work with you to:
Most people begin to notice meaningful changes within 6 to 12 sessions. Some people benefit from fewer. Others with more complex or long-standing difficulties benefit from a longer course. Your psychologist will work with you to find the pace and depth that fits your situation.
It is not magic. It is skill building. And like any skill, it becomes more natural with practice.
Yes. Research consistently shows that CBT delivered via secure video is as effective as face-to-face sessions for the majority of conditions, including anxiety, depression, and insomnia.
At Chrysalis, we offer telehealth CBT sessions for clients anywhere in Australia, including regional and rural areas where access to psychology services is limited. All you need is a private space, a device with a camera, and a stable internet connection.

.svg)
CBT is often used as a standalone treatment, but at Chrysalis our psychologists may integrate it with other evidence-based approaches depending on your needs. These include EMDR for trauma processing, Acceptance and Commitment Therapy (ACT), Dialectical Behaviour Therapy (DBT), Schema Therapy, and Compassion Focused Therapy (CFT).
Your psychologist will work with you to find the combination that best fits your situation and goals.
You do not need a diagnosis to start. You do not need to be in crisis. You just need to be ready to take one step.
Whether you are in Hobart, regional Tasmania, or anywhere else in Australia, support is available. Our psychologists are ready to help.
At Chrysalis Psychology & Wellbeing, our psychologists are trained in CBT and ready to help.
Phone: (03) 6263 6319
Email: info@chrysalispsychwell.com.au
Website: www.chrysalispsychwell.com.au
Knopwood House, Level 2, 38 Montpelier Retreat, Battery Point, Tasmania 7004
Face-to-face in Battery Point, Hobart. Telehealth across Australia.
.svg)
“Why Am I Always Tired? A Psychologist's Guide to Understanding Exhaustion”
"When Trauma Gets Stuck: How EMDR Therapy Helps"- Read our blog posts.
Australian Psychological Society (2018). Evidence-based psychological interventions in the treatment of mental disorders: A review of the literature (4th ed.). Melbourne: APS.
Cuijpers, P., Miguel, C., Harrer, M., Plessen, C.Y., Ciharova, M., Ebert, D., & Karyotaki, E. (2023). Cognitive behavior therapy vs. control conditions, other psychotherapies, pharmacotherapies and combined treatment for depression: a comprehensive meta-analysis including 409 trials with 52,702 patients. World Psychiatry, 22(1), 105-115.
Fordham, B., Sugavanam, T., Edwards, K., et al. (2021). The evidence for cognitive behavioural therapy in any condition, population or context: a meta-review of systematic reviews and panoramic meta-analysis. Psychological Medicine, 51(1), 21-29.
Hofmann, S.G., Asnaani, A., Vonk, I.J.J., Sawyer, A.T., & Fang, A. (2012). The efficacy of cognitive behavioral therapy: a review of meta-analyses. Cognitive Therapy and Research, 36(5), 427-440.
Meine, L.E., Weber, M.C., et al. (2024). A systematic review and meta-analysis of transdiagnostic cognitive behavioural therapies for emotional disorders. Nature Human Behaviour.
World Health Organisation (2022). World mental health report: transforming mental health for all. Geneva: WHO.